- Thu. Apr 18th, 2024
Latest Post
Extraordinary Memories: The Science Behind Highly Superior Autobiographical Memory (HSAM) and Its Implications for Understanding Brain Function
People possessing the ability to accurately recall events from any given day of their lives are known as individuals with Highly Superior Autobiographical Memory (HSAM). This rare phenomenon typically manifests…
Penn State Health Goes Green: Installs Electric Vehicle Charging Stations at Three Hospitals for EV Owners
Penn State Health has installed electric vehicle (EV) charging stations at three of its hospitals to accommodate patients, visitors, employees, and students who drive EVs. Hampden Medical Center has eight…
Zuckerberg Surpasses Musk as World’s Third-Richest Person, Boosted by Meta Platforms Stock Performance
Elon Musk has been surpassed by Mark Zuckerberg to become the world’s third-richest person, with a fortune of $175 billion. This year, Zuckerberg has seen an increase of $47 billion…
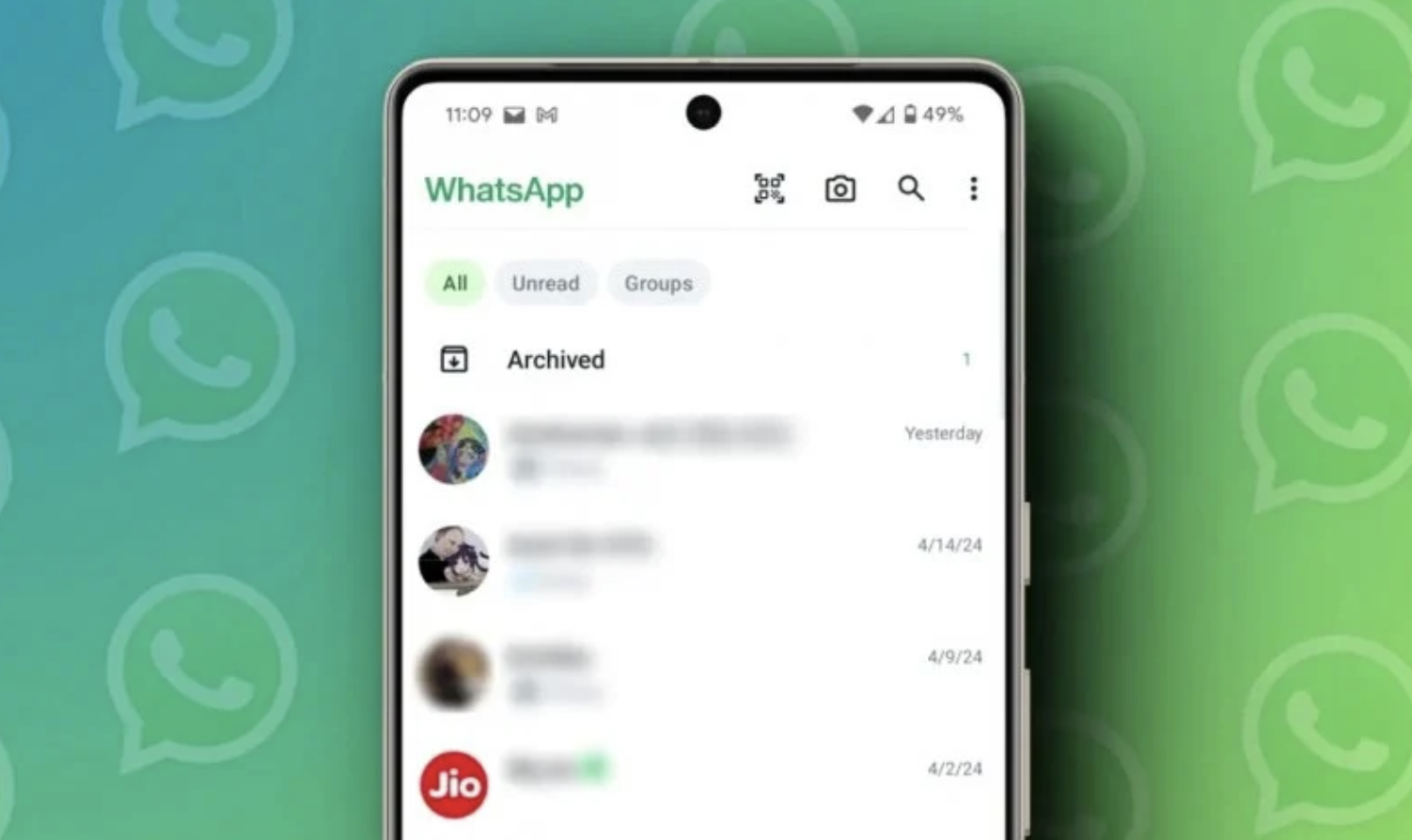
Filter Your Way to Better Conversation Management with WhatsApp’s New Chat Filters
WhatsApp, the popular messaging app from Meta, has recently introduced a new feature to improve the organization and accessibility of the user interface. The app has launched “chat filters,” which…
Kennedys’ Unwavering Support for Biden: A Family Legacy of Unity and Service in Politics”.
The Kennedy family has a long history of political involvement and their loyalty to the Democratic Party runs deep. While many members of the family have publicly endorsed President Joe…
Global Concerns for Globetronics Technology Bhd: Financial Results and Future Outlook
In 2023, Globetronics Technology Bhd (KLSE:GTRONIC) reported its full-year financial results, showing a decrease in revenue to RM131.8m, down 27% from the previous year. Net income also decreased by 42%…
Unearthing the Past: The Mysterious Horseshoe-Shaped Monument in Marliens, France
In Marliens, a commune in eastern France, archaeologists have made an intriguing discovery. The site, which dates back to various historical periods, features a horseshoe-shaped monument and a variety of…
MENA Region Economic Outlook: A Return to Low Growth Rates Amid Slowing Global Economy
In 2024, the Middle East and North Africa (MENA) region is expected to grow by 2.7%, marking a return to the low growth rates that prevailed in the decade before…
250,000 Deaths and $4 Billion in Health Costs: The Urgent Need for Action on Climate Change and its Impact on Public Health
In the coming decades, climate change will lead to an estimated 250,000 additional deaths annually worldwide due to malnutrition, malaria, diarrhea, and heat stress. Additionally, the direct health costs associated…
Albany Business Owners Call for Stronger Penalties in Fight Against Property Crimes
Business owners in Albany are raising concerns over the rise in property crimes in the area. Dougherty County District Attorney Greg Edwards is addressing these concerns and notes that some…